Are operating rooms sterile
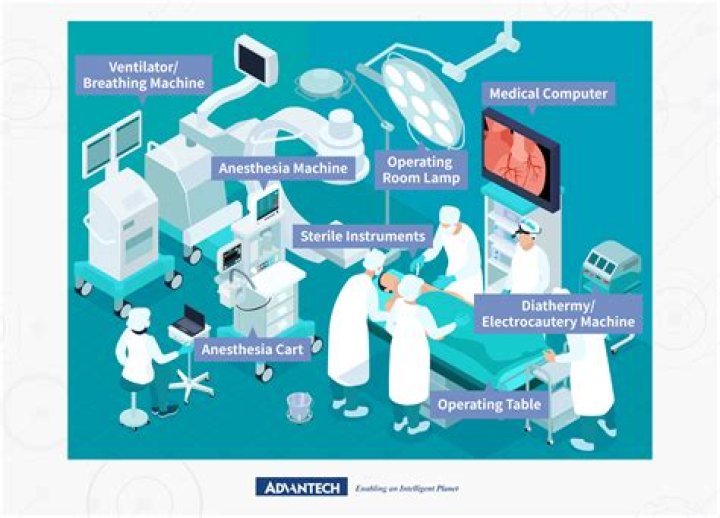
The operating room (OR) is a sterile, organized environment. As a health care provider, you may be required to enter the OR during a surgical procedure or to set up before a surgical procedure.
How do operating rooms maintain sterility?
Maintain a safe space or margin of safety between sterile and non-sterile objects and areas. Refrain from reaching over the sterile field. Keep operating room (OR) traffic to a minimum, and keep doors closed. Keep hair tied back.
What are the sterile fields in the operating room?
A sterile field is an area created by placing sterile surgical drapes around the patient’s surgical site and on the stand that will hold sterile instruments and other items needed during surgery.
When did operating rooms become sterile?
Believe it or not, this was a common scenario little more than a century ago—until 1888, when Johnson & Johnson helped introduce the concept of sterile surgery by publishing a first-of-its-kind educational manual, Modern Methods of Antiseptic Wound Treatment, which explained how to prevent the spread of infection- …Are operating rooms clean rooms?
The operating rooms are known as clean rooms because it must have the high quality air without the dust and the particles. In the clean room, the dust that is sourced from both the personnel and the patient and the machines, causes the risk of infection.
What is sterile OT?
OT should be divided into four zones named protective, clean, aseptic and disposal zones. … Steps for maintaining sterile environment include cleaning and disinfection of operation theatres by various means like chemical disinfection or disinfection with ultraviolet radiation.
Why is sterility important in the operating room?
The purpose of creating a sterile field is to reduce the number of microbes present to as few as possible. The sterile field is used in many situations outside the operating room as well as inside the operating room when performing surgical cases.
When did doctors start sterilizing?
Two major contributions to the art of sterilization came in the 1860’s when the French chemist and microbiologist Louis Pasteur wrote extensively on how germs cause disease and the English physician, Joseph Lister, developed a technique that used carbolic acid as a spray to disinfect instruments.How do surgeons sterilize their tools?
Steam or autoclave sterilization is the most common method of instrument sterilization. Instruments are placed in a surgical pack and exposed to steam under pressure. A sterilization indicator (required) such as autoclave tape or an indicator strip is used to identify instruments that have been sterilized.
Why do surgeons scrub before surgery?In summary, the purposes of the surgical scrub and surgical attire is to promote patient safety by helping to prevent environmental contamination; prevent the transfer of transient microorganisms and debris from the hands and forearms; decrease the number of resident microorganisms to an irreducible minimum; and …
Article first time published onCan you reach over a sterile field?
Refrain from reaching over the sterile field. Keep operating room (OR) traffic to a minimum, and keep doors closed. Keep hair tied back. When pouring sterile solutions, only the lip and inner cap of the pouring container is considered sterile.
Which member of the OR team is sterile?
2. Scrub nurse. For all surgical procedures there is a sterile member called the scrub nurse or surgical technologist to organize the instruments and pass it to the surgeon when needed. He or she is in the charge of the Mayo stand (the sterile tray with the instruments).
Who cleans the operating room?
High-Touch Surfaces: Perform assessments and observations of workflow in consultation with clinical staff in each patient care area to determine key high-touch surfaces. Include identified high-touch surfaces and items in checklists and other job aids to facilitate completing cleaning procedures. See 2.4.
How often should an operating room be cleaned?
Every operating room should be terminally cleaned when the scheduled procedures are complete for the day or once during each 24 hour period during regular hours of operation (regular hours of operation are defined by facility).
Is there extra oxygen in operating rooms?
Surgical areas are oxygen-enriched environments and especially susceptible to fires due to the use of supplemental oxygen and nitrous oxide. In this environment, materials that do not ordinarily burn in air may ignite, and those that do burn in air will burn hotter and faster.
What are methods of sterilization?
Sterilization can be achieved by a combination of heat, chemicals, irradiation, high pressure and filtration like steam under pressure, dry heat, ultraviolet radiation, gas vapor sterilants, chlorine dioxide gas etc.
Can hair sterilized?
The results of our study demonstrate that hair, silk suture, and nylon suture can be rendered free from pathogenic activity by sterilization because there was no growth from all 3 items after processing. Sterilization is the process that kills all types of microorganisms, including bacterial spores.
What are the 5 principles of sterile technique?
- Face to face or back to back.
- Turn back to a non-sterile person or when passing.
- Face a sterile area when passing the area.
- Ask a non-sterile person to step aside rather than trying to crowd past him.
- Step back away from the sterile field to sneeze or cough.
How do you sterilize an operating Theatre?
- Place a cautionary ‘Wet Floor’ sign at the entrance of the room.
- Prepare fresh hospital approved disinfectant solution according to manufacturer’s instructions.
- Clean hands and put on gloves.
- Collect and remove waste.
- Collect and remove all soiled linen.
How will you sterilize an operation Theatre?
Sterilization is carried out most commonly using steam sterilizers or ethylene dioxide sterilizers. The waste generated during practice is a potential source of nosocomial infections and should be treated as per the proper protocol and guidelines. Trained staff to carry out these practices is essential.
Why Operation Theatre is sterilized?
Sterilization means eradicating germs completely, which is not 100% possible in an operation theater. The sources of bacterial contamination are from air and the environment, infected body fluids, patients, articles, equipment etc.
Do hospitals reuse surgical tools?
As a rule, if there is a risk of infection, he chooses disposable instruments. However, many surgeons still reuse equipment to reduce overhead costs in an ambulatory surgical center (ASC) setting. … If they are using stainless steel, they tend to sterilize and reuse.
How are hospitals sterilized?
By far, the industry standard for sterilization today is to use pressurized high-temperature steam to kill all microorganisms in a specialized machine called an autoclave. Based on the model of the pressure-cooker, modern autoclaves run various cycles for different types of equipment and materials, as well as liquids.
Does surgical equipment get reused?
Reusable medical devices are devices that health care providers can reprocess and reuse on multiple patients. Examples of reusable medical devices include surgical forceps, endoscopes and stethoscopes. … Critical devices, such as surgical forceps, come in contact with blood or normally sterile tissue.
What are the 3 types of sterilization?
- Plasma Gas Sterilizers. …
- Autoclaves. …
- Vaporized Hydrogen Peroxide Sterilizers.
What was Joseph Lister's big breakthrough?
Lister successfully introduced carbolic acid (now known as phenol) to sterilise surgical instruments and to clean wounds. Applying Louis Pasteur’s advances in microbiology, Lister championed the use of carbolic acid as an antiseptic, so that it became the first widely used antiseptic in surgery.
What is flash sterilization in dentistry?
Flash sterilization is a method for sterilizing unwrapped patient-care items for immediate use. The time required depends on the type of sterilizer and the type of instrument (i.e., porous or nonporous) to be sterilized (Table 3).
Why don t surgeons put their own gloves on?
Sterile surgical gloves were wiped over the surface of a lead hand. … Significant amount of lead is transferred on to the gloves after handling a lead hand. This risks wound contamination and a foreign body reaction. Covering the lead hand with a sterile drape may minimise the risk of surgical wound contamination.
Why do doctors keep their hands up?
Why do surgeons put their hands up after scrubbing? Surgical scrubbing is the removal of the germs and bacteria as possible from the bare hands and arms. After scrubbing, keep both hands above waist and below neckline. … Scrubbed hands and arms are considered contaminated once they fall below waist level.
Why do surgeons scrub their hands if they wear gloves?
Surgical gloves prevent contact with bodily fluids during procedures. This prevents contamination for the patient and the surgeon. This reduces viral and bacterial transmission. Glove tears do happen and having clean hands reduces the chance for surgeon to patient transmission and cross contamination between patients.
What happens if you break sterile field?
A break in sterility can result in infection and seriously harm the patient. Each year 1.7 million patients acquire a healthcare-associated infection (HAI) and almost 100,000 of them die. At least one in five of these infections could have been prevented.