What are the phases of Aki
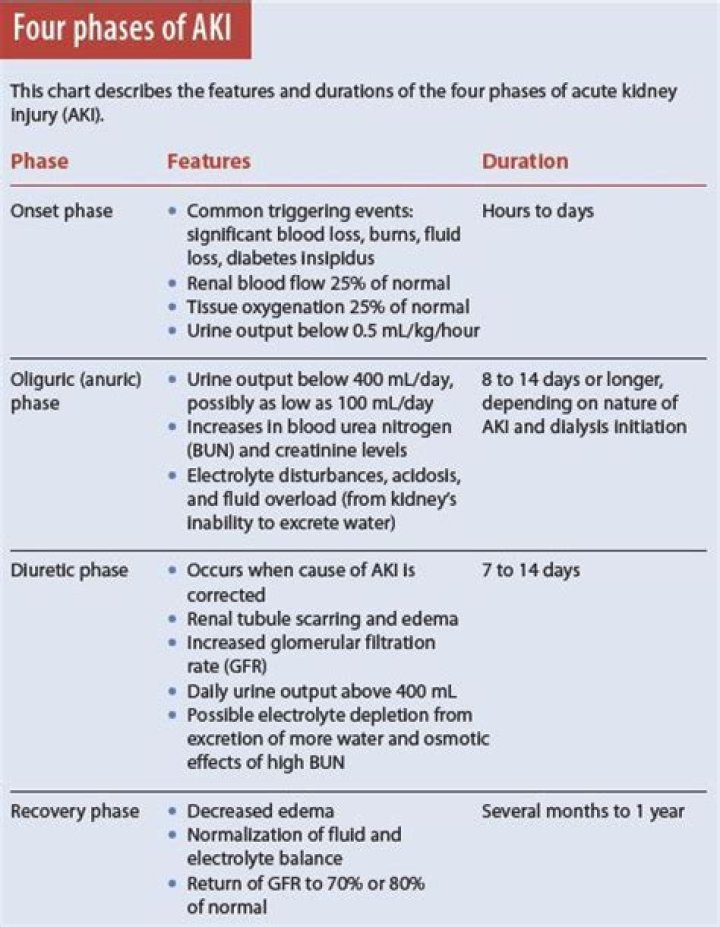
Onset phase: Kidney injury occurs.Oliguric (anuric) phase: Urine output decreases from renal tubule damage.Diuretic phase: The kidneys try to heal and urine output increases, but tubule scarring and damage occur.Recovery phase: Tubular edema resolves and renal function improves.
How many stages are there in Aki?
The severity of AKI is described by categorising into three stages, with stage 1 being the least severe and stage 3 being the most severe (see Box 1).
What are the three phases of acute tubular necrosis?
- Onset or initiating phase. Lasting hours or days, this is the time from onset of the precipitating event (for example, toxin exposure) until tubular injury occurs.
- Maintenance phase. …
- Recovery phase.
What are the three types of Aki?
The causes of acute kidney injury can be divided into three categories (Table 29): prerenal (caused by decreased renal perfusion, often because of volume depletion), intrinsic renal (caused by a process within the kidneys), and postrenal (caused by inadequate drainage of urine distal to the kidneys).What is the first phase of acute renal failure?
The initiation phase of ATN occurs when renal blood flow (RBF) decreases to a level resulting in severe cellular ATP depletion that in turn leads to acute cell injury and dysfunction. Renal tubular epithelial cell injury is a key feature of the Initiation Phase (532).
What are the 5 stages of kidney failure?
Stages of CKDGFR in mL/minStatus of kidney functionStage 260-89A mild decline in kidney functionStage 330-59A moderate decline in kidney functionStage 415-29A severe decline in kidney functionStage 5<15Kidney failure or end-stage renal disease (ESRD) requiring dialysis
What is pathophysiology of AKI?
The pathophysiology of AKI involves a complex interplay among vascular, tubular, and inflammatory factors followed by a repair process that can either restore epithelial differentiation and function to normal or result in fibrotic chronic kidney disease.
What causes Intrarenal AKI?
The most common causes of nonoliguric AKI are acute tubular necrosis (ATN), aminoglycoside nephrotoxicity, lithium toxicity, and cisplatin nephrotoxicity.What is Intrarenal AKI?
Intrinsic or intrarenal acute kidney injury (AKI) , which used to be called acute renal failure, occurs when direct damage to the kidneys causes a sudden loss in kidney function. The treatment of intrinsic acute kidney injury includes identifying and correcting the cause of the kidney injury.
What does AKI Stage 0 mean?AKI stage 0 No comment because the serum creatinine has not changed significantly. AKI Stage NA. Insufficient data. No serum creatinine within 1 year. Serum creatinine within reference.
Article first time published onWhat is septic ATN?
Acute tubular necrosis (ATN) is classically used to describe the cellular effects of sepsis driven by both ischemia-reperfusion injury and cytokine-mediated inflammation.
What is ischemic ATN?
ATN may be classified as either toxic or ischemic. Toxic ATN occurs when the tubular cells are exposed to a toxic substance (nephrotoxic ATN). Ischemic ATN occurs when the tubular cells do not get enough oxygen, a condition that they are highly sensitive and susceptible to, due to their very high metabolism.
What is a uremic patient?
Uremia is a dangerous condition that occurs when waste products associated with decreased kidney function build up in your blood. Uremia means “urine in the blood” and refers to the effects of the waste product accumulation. It affects the entire body.
What is the diuretic phase of Aki?
Diuretic Phase: In this phase, daily urine output is approximately 1 to 3 liters but can reach as high as 5 liters or more. The kidneys recover their ability to excrete waste but cannot concentrate the urine. Hypovolemia and hypotension may occur due to massive volume loss.
What is Polyuric phase of Aki?
In the polyuric phase of AKI, potassium and phosphorus may be depleted, so that patients may require dietary supplementation and IV replacement. Calculation of the nitrogen balance can be challenging, especially in the presence of volume contraction, hypercatabolic states, GI bleeding, and diarrheal disease.
Why is Bun elevated in Aki?
Volume depletion, hyperalimentation, gastrointestinal bleeding, and exogenous glucocorticoids raise BUN and are seen commonly in AKI patients in critical care settings.
What are the 4 stages of kidney failure?
Stage 2 Mild CKD (GFR = 60-89 mL/min) Stage 3A Moderate CKD (GFR = 45-59 mL/min) Stage 3B Moderate CKD (GFR = 30-44 mL/min) Stage 4 Severe CKD (GFR = 15-29 mL/min)
How many stages are there in kidney failure?
There are five stages of chronic kidney disease. The mildest are stages 1 and 2. In these early stages of kidney disease, the kidneys are damaged and not working at full strength. At stage 3, about half of kidney function has been lost.
What does a GFR of 53 mean?
A GFR of 60 or higher is in the normal range. A GFR below 60 may mean kidney disease. A GFR of 15 or lower may mean kidney failure.
What lab values indicate AKI?
Accordingly, AKI is diagnosed if serum creatinine increases by 0.3 mg/dl (26.5 μmol/l) or more in 48 h or rises to at least 1.5-fold from baseline within 7 days (Table 1). AKI stages are defined by the maximum change of either serum creatinine or urine output.
Is ATN Prerenal or Intrarenal?
Prerenal: decreased renal perfusion (often from hypovolemia) leading to a decrease in GFR; reversible. Intrarenal: intrinsic kidney damage; ATN most common due to ischemic/nephrotoxic injury. Postrenal: extrinsic/intrinsic obstruction of the urinary collection system.
What is the difference between Prerenal Intrarenal and Postrenal?
Pre-renal, generally in which decreased renal blood flow results in a drop in GFR. Intrinsic/intra-renal, in which a disease process causes damage to the kidney itself. Post-renal, in which a process downstream of the kidney prevents drainage of urine (urinary tract obstruction)
What is Intrarenal azotemia?
Intrarenal azotemia. Intrarenal azotemia, also known as acute kidney injury (AKI), renal-renal azotemia, and (in the past) acute renal failure (ARF), refers to elevations in BUN and creatinine resulting from problems in the kidney itself.
What is Stage 3 AKI CKD?
Stage 3 CKD means you have an eGFR between 30 and 59. An eGFR between 30 and 59 means that there is some damage to your kidneys and they are not working as well as they should.
What happens when kidneys start to shut down?
If your kidneys stop working completely, your body fills with extra water and waste products. This condition is called uremia. Your hands or feet may swell. You will feel tired and weak because your body needs clean blood to function properly.
What is Aki warning stage1?
As a guide: If AKI warning stage 1 (current creatinine 1.5 or more times the baseline level or creatinine rise more than 26 micromol/L or greater within 48 hours) and there is a: Low pre-test probability of AKI (stable clinical context), consider clinical review within 72 hours of the result.
What is difference between AKI and ATN?
Acute tubular necrosis (ATN) is the most common cause of acute kidney injury (AKI) in the renal category (that is, AKI in which the pathology lies within the kidney itself). The term ATN is actually a misnomer, as there is minimal cell necrosis and the damage is not limited to tubules.
What type of AKI is sepsis?
Thus, S-AKI is usually defined as AKI in the presence of sepsis without other significant contributing factors explaining AKI or characterized by the simultaneous presence of both Sepsis-3 and Kidney Disease: Improving Global Outcomes (KDIGO) criteria.
What is pre renal azotemia?
Prerenal azotemia is the most common form of kidney failure in hospitalized people. Any condition that reduces blood flow to the kidney may cause it, including: Burns. Conditions that allow fluid to escape from the bloodstream. Long-term vomiting, diarrhea, or bleeding.
What is ATI kidney?
Acute tubular injury (ATI) is the new nomenclature, now commonly used in place of acute tubular necrosis to define a sudden reduction in renal functioning, resulting from a myriad of different insults to the renal tubular epithelial cells.
What is GFR test?
A glomerular filtration rate (GFR) is a blood test that checks how well your kidneys are working. Your kidneys have tiny filters called glomeruli. These filters help remove waste and excess fluid from the blood. A GFR test estimates how much blood passes through these filters each minute.



