What are the phases of ARDS
In ARDS, the injured lung is believed to go through three phases: exudative, proliferative, and fibrotic, but the course of each phase and the overall disease progression is variable.
What occurs first in ARDS?
In the early stages of ARDS, fluid from the smallest blood vessels in the lungs starts to leak into the alveoli—the tiny air sacs where oxygen exchange takes place. The lungs become smaller and stiffer and it becomes hard to breath. The amount of oxygen in the blood falls. This is called hypoxemia.
What is the hallmark of ARDS?
Acute respiratory distress syndrome (ARDS) is a diffuse inflammatory reaction of the lung to an insult and is characterized by increased pulmonary capillary permeability, lung edema, and atelectasis. The histological hallmark of ARDS is diffuse alveolar damage and its pathognomonic hyaline membranes.
What is the disease process of ARDS?
Acute respiratory distress syndrome (ARDS) occurs when fluid builds up in the tiny, elastic air sacs (alveoli) in your lungs. The fluid keeps your lungs from filling with enough air, which means less oxygen reaches your bloodstream. This deprives your organs of the oxygen they need to function.What is the fibrotic stage of ARDS?
Interstitial and intra-alveolar fibrosis are hallmarks of the more advanced stages of ARDS and are characterised by the abnormal and excessive deposition of extracellular matrix proteins, in particular collagen.
Can ARDS be seen on xray?
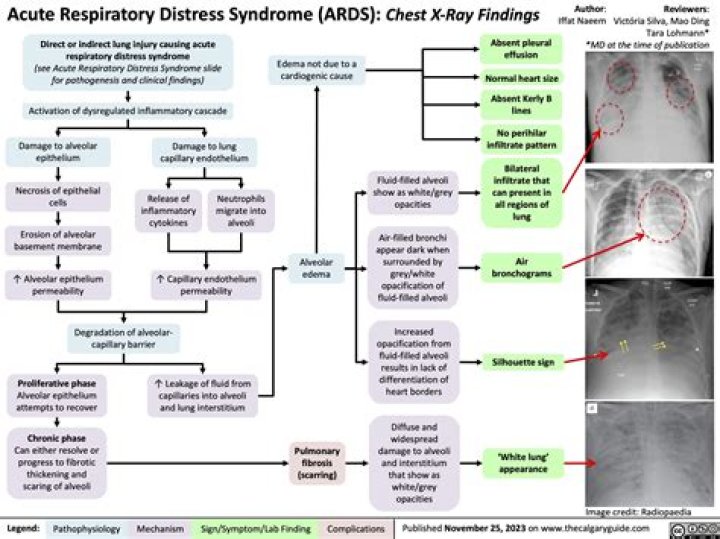
Chest radiograph findings of ARDS vary widely depending on the stage of the disease. The most common chest radiograph findings are bilateral, predominantly peripheral, somewhat asymmetrical consolidation with air bronchograms. Septal lines and pleural effusions, however, are uncommon.
What is the acute phase of ARDS?
The acute phase of ARDS is characterised by injury to the alveolar–capillary barrier, with disruption leading to increased permeability (‘leakiness’). Leukocytes accumulate in the pulmonary capillaries and invade the airspaces.
How long does Covid ARDS last?
Lasting effects can include: Difficulty breathing. It can take up to two years for people recovering from ARDS to regain lung function. A physical therapist can help patients maximize their lung capacity.What is Peep measured in?
This pressure is typically achieved by maintaining a positive pressure flow at the end of exhalation. This pressure is measured in centimeters of water.
How do you treat ARDS patients?- Ventilator support. All patients with ARDS will require extra oxygen. …
- Prone positioning. ARDS patients are typically in bed on their back. …
- Sedation and medications to prevent movement. …
- Fluid management. …
- Extracorporeal membrane oxygenation (ECMO) …
- For More Information:
What are the diagnostic criteria for ARDS?
The American-European Consensus Conference (AECC) has published diagnostic criteria for ARDS: acute onset; ratio of partial pressure of arterial oxygen to fraction of inspired oxygen (PaO2/FiO2) of 200 or less, regardless of positive end-expiratory pressure; bilateral infiltrates seen on frontal chest radiograph; and …
How do you calculate severity in ARDS?
The severity of the ARDS is defined by the degree of hypoxemia, which is calculated as the ratio of arterial oxygen tension to fraction of inspired oxygen (PaO2/FiO2).
What does a low PF ratio mean?
The P/F ratio equals the arterial pO2 (“P”) from the ABG divided by the FIO2 (“F”) – the fraction (percent) of inspired oxygen that the patient is receiving expressed as a decimal (40% oxygen = FIO2 of 0.40). A P/F Ratio less than 300 indicates acute respiratory failure.
Which phase of ARDS is characterized by the accumulation of excessive fluid protein and inflammatory cells in the alveoli?
The acute phase of acute lung injury (ALI) and the acute re- spiratory distress syndrome (ARDS) are characterized by the influx of protein-rich edema fluid into the alveolar spaces as a consequence of increased permeability of the alveolar-capil- lary barrier.
Whats the difference between ARF and ARDS?
Acute respiratory failure (ARF) is a term often used alongside ARDS, but it is a broader term that refers to the failure of the lungs from any causes, such as chronic obstructive pulmonary disease (COPD).
What is ALI and ARDS?
Acute respiratory distress syndrome (ARDS), and its milder form acute lung injury (ALI), are a spectrum of lung diseases characterised by a severe inflammatory process causing diffuse alveolar damage and resulting in a variable degree of ventilation perfusion mismatch, severe hypoxaemia, and poor lung compliance.
What is the pathophysiology of RDS?
PATHOPHYSIOLOGY: The primary cause of RDS is inadequate pulmonary surfactant. The structurally immature and surfactant-deficient lung has ↓ compliance and a tendency to atelectasis; other factors in preterm infants that ↑ the risk of atelectasis are decreased alveolar radius and weak chest wall.
What is a hyaline membrane in ARDS?
Diffuse alveolar damage (DAD): an acute lung condition with the presence of hyaline membranes. These hyaline membranes are made up of dead cells, surfactant, and proteins. The hyaline membranes deposit along the walls of the alveoli, where gas exchange typically occurs, thereby making gas exchange difficult.
Is ARDS respiratory acidosis or alkalosis?
In addition to hypoxemia, arterial blood gases often initially show a respiratory alkalosis. However, in ARDS occurring in the context of sepsis, a metabolic acidosis with or without respiratory compensation may be present.
What are complications of ARDS?
ARDS may take several days to develop, or it can rapidly get worse. Complications may include blood clots, infections, additional lung problems, or organ failure.
Which is part of the nursing management for ARDS?
Managing patients with ARDS requires maintaining the airway, providing adequate oxygenation, and supporting hemodynamic function. The five P’s of supportive therapy include perfusion, positioning, protective lung ventilation, protocol weaning, and preventing complications.
What does a PEEP of 5 mean?
A higher level of applied PEEP (>5 cmH2O) is sometimes used to improve hypoxemia or reduce ventilator-associated lung injury in patients with acute lung injury, acute respiratory distress syndrome, or other types of hypoxemic respiratory failure.
What is FIO2 and PEEP?
Initial Adult Ventilator Settings. You have to start somewhere ✓ Fraction of inspired oxygen (FiO2)—100% ✓ Positive End Expiratory Pressure (PEEP)–5 cmH20 ✓ Respiratory Rate—12 breaths per minute ✓ Tidal Volume 6-8 ml per weight in kilograms (ideal body weight). Most adults will require at least 500 ml.
What is the highest PEEP level?
Under controlled conditions, higher levels of PEEP are well tolerated. PEEP of 29 appears to be the highest tolerated PEEP in our patient. We noted an initial rise in blood flow across all cardiac valves followed by a gradual decline.
What are the chances of surviving ARDS?
Though there is no cure for ARDS, it’s not uniformly fatal. With treatment, an estimated 60% to 75% of those who have ARDS will survive the disease.
How do I know if pneumonia is gone?
- 1 week – high temperature should have gone.
- 4 weeks – chest pain and mucus production should have substantially reduced.
- 6 weeks – cough and breathlessness should have substantially reduced.
- 3 months – most symptoms should have resolved, but you may still feel very tired (fatigue)
What is the mortality rate of ARDS?
ARDS is associated with appreciable mortality, with the best estimates from a multicenter, international cohort study of 3022 patients with ARDS, suggesting an overall rate of death in the hospital of approximately 40 percent [1-4].
How long can a person be on a ventilator in an ICU?
Some people may need to be on a ventilator for a few hours, while others may require one, two, or three weeks. If a person needs to be on a ventilator for a longer period of time, a tracheostomy may be required.
Can lungs heal on a ventilator?
This is done only if your health care team believes that it would take longer than 2 weeks to remove you from the ventilator. A tracheostomy isn’t permanent and can easily be removed once you no longer need the ventilator. It’s important to note that even in people with severe lung damage, the lung can heal.
What accounts for the severe hypoxia associated with ARDS?
- Elevated alveolar capillary hydrostatic pressure, as occurs in left ventricular failure. …
- Increased alveolar capillary permeability, as occurs in any of the conditions predisposing to acute respiratory distress syndrome (ARDS)
- Blood (as occurs in diffuse alveolar hemorrhage.
Why is Pcwp normal in ARDS?
A normal PCWP (less than 18 mm Hg) helps to distinguish ARDS from left atrial hypertension, a condition in which PCWP is elevated.



