What is surfactant in lungs
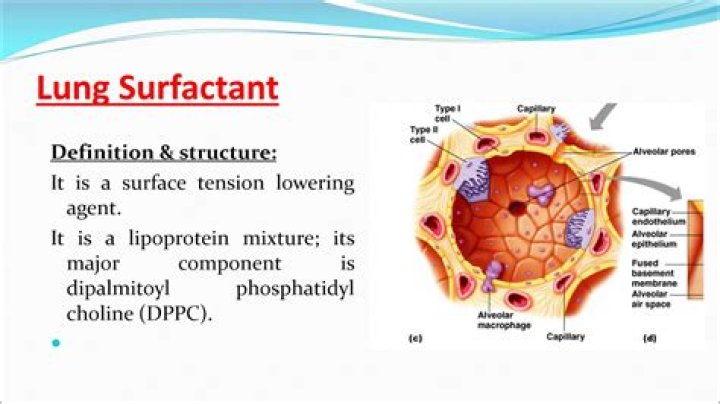
Pulmonary surfactant is essential for life as it lines the alveoli to lower surface tension, thereby preventing atelectasis during breathing. … The hydrophobic proteins, SP-B and SP-C, together with dipalmitoylphosphatidylcholine, confer surface tension-lowering properties to the material.
What is the role of surfactant in the lung?
Pulmonary surfactant is essential for life as it lines the alveoli to lower surface tension, thereby preventing atelectasis during breathing. … The hydrophobic proteins, SP-B and SP-C, together with dipalmitoylphosphatidylcholine, confer surface tension-lowering properties to the material.
Why surfactant is important?
The main function of surfactant is to lower the surface tension at the air/liquid interface within the alveoli of the lung. This is needed to lower the work of breathing and to prevent alveolar collapse at end-expiration.
What causes lack of surfactant in lungs?
Surfactant dysfunction is caused by mutations in one of several genes, including SFTPB, SFTPC, and ABCA3. Each of these genes is involved in the production of surfactant. The production and release of surfactant is a complex process.What are surfactants in respiratory system?
Surfactant is an agent that decreases the surface tension between two media. The surface tension between gaseous-aqueous interphase in the lungs is decreased by the presence of a thin layer of fluid known as pulmonary surfactant. The pulmonary surfactant is produced by the alveolar type-II (AT-II) cells of the lungs.
Where is surfactant located in the lungs?
Pulmonary surfactant is a complex and highly surface active material composed of lipids and proteins which is found in the fluid lining the alveolar surface of the lungs.
Is surfactant a medicine?
Pulmonary surfactant is used as a medication to treat and prevent respiratory distress syndrome in newborn babies. Prevention is generally done in babies born at a gestational age of less than 32 weeks. It is given by the endotracheal tube. Onset of effects is rapid.
How is surfactant deficiency diagnosed?
Surfactant Protein B (SP-B) Deficiency It is an autosomal recessive condition. Infants present shortly after birth with respiratory distress and failure, despite assisted ventilation and surfactant replacement therapy. The diagnosis is made by genetic testing for the mutation in the child and both parents.Do adults have surfactant?
Surfactant deficiency in adults with acute respiratory distress syndrome has long been recognized. Although clinical trials of surfactant therapy in adults have not achieved the level of success seen in neonates, multiple recent trials have suggested that success is possible.
What are the side effects of surfactant?The short-term risks of surfactant replacement therapy include bradycardia and hypoxemia during instillation, as well as blockage of the endotracheal tube (36).
Article first time published onWhat is given to increase surfactant?
The steroids stimulate (via the fibroblast-pneumonocyte factor) production of surfactant phospholipids by alveolar type II cells, enhance the expression of surfactant-associated proteins, reduce microvascular permeability, and accelerate overall structural maturation of the lungs.
How is surfactant given?
Methods to deliver surfactant The surfactant is administered via a thin catheter into the trachea in small aliquots, while the baby is spontaneously breathing on CPAP support. In infants 29-32 weeks gestation, LISA may reduce the occurrence of pneumothorax and need for mechanical ventilation.
How do you increase the surfactant?
Surfactant secretion can be stimulated by a number of mechanisms. Type II cells have beta-adrenergic receptors and respond to beta-agonists with increased surfactant secretion [40]. Purines, such as adenosine triphosphate are potent stimulators of surfactant secretion and may be important for its secretion at birth.
What does surfactant mean?
surfactant, also called surface-active agent, substance such as a detergent that, when added to a liquid, reduces its surface tension, thereby increasing its spreading and wetting properties.
How does surfactant reduce lung recoil?
The work required to separate contiguous alveolar walls is directly proportional to the surface tension of the fluid lining. By reducing the surface tension of the alveolar hypophase, pulmonary surfactant greatly reduces the work required to initiate lung inflation.
Who created surfactant?
The story of surfactant probably began in 1929 when Kurt von Neergaard, a German-born Physiologist working in Switzerland filled a porcine lung with an isotonic gum solution ‘to eliminate surface tension of the air tissue interfaces’.
What antibiotics treat ARDS?
Antimicrobials were prescribed in all the patients, as majority of the cases of ARDS were secondary to an infectious aetiology. The beta lactam antibiotics were the most commonly prescribed antimicrobials followed by doxycycline.
Where does surfactant come from?
Surfactant is produced exclusively by alveolar type II epithelial cells and stored in specialized organelles called lamellar bodies (LBs) until it is secreted into the lumen of the alveolus. Secreted surfactant is recycled by type II cells to be repackaged and secreted again.
How is pulmonary surfactant produced?
Pulmonary surfactant is a complex mixture of phospholipids, neutral lipids, and specific proteins; it is produced by the alveolar type II epithelial cell (AEC2), stored in intracellular organelles known as lamellar bodies, and secreted by exocytosis into the alveolar lumen.
What happens to surfactant in pneumonia?
In pneumonia, bacteria induce changes in pulmonary surfactant. These changes are mediated by bacteria directly on secreted surfactant or indirectly through pulmonary type II epithelial cells.
What happens to surfactant in COPD?
COPD patients showed significant alterations in their surfactant lipidomes and exhibited an overall decrease in alveolar total lipid availability that directly correlated with decreased pulmonary function.
What is false surfactant?
What is false about surfactant? Surfactant increases the surface tension of water. Surfactant causes water to form a thin sheet instead of a bead. Surfactant reduces the chance the alveoli walls collapsing on each other.
Which situation will happen when you have emphysema?
In emphysema, the inner walls of the lungs’ air sacs (alveoli) are damaged, causing them to eventually rupture. This creates one larger air space instead of many small ones and reduces the surface area available for gas exchange. Emphysema is a lung condition that causes shortness of breath.
How does smoking affect the surfactant layer?
However, it is not clear what effect smoke has on the surfactant. Most studies have demonstrated that smoking reduces bronchoalveolar lavage phospholipid levels. Some components of smoke also appear to have a direct detergent-like effect on the surfactant while others appear to alter cycling or secretion.
What would happen in a disease state in which there is no surfactant How would Compliance change what would happen to the alveoli?
The surfactant reduces surface tension within all alveoli through hydrophilic and hydrophobic forces. Insufficient pulmonary surfactant in the alveoli can contribute to atelectasis (collapse of part or all of the lung ).
How late can surfactant be given?
Ideally the dose should be given within 1 hr of birth but definitely before 2 hours of age. A repeat dose should be given within 4 – 12 hours if the patient is still intubated and requiring more than 30 to 40% oxygen.
What age can you give surfactant?
1 For infants intubated immediately after birth, it is recommended that surfactant be given as early treatment (<2 h of age), except if the infant is on room air and minimal ventilatory support on neonatal intensive care unit admission.
How do you give survanta?
- Slowly withdraw the entire contents of the vial into a plastic syringe through a large-gauge needle (e.g., at least 20 gauge).
- Attach the premeasured 5 French end-hole catheter to the syringe. …
- When administering SURVANTA using a 5 French end-hole catheter, administer in four quarter-dose aliquots.
How does betamethasone increase surfactant?
Respiratory Disorders in the Newborn Antenatal steroids that cross the placenta (i.e., synthetic steroids such as dexamethasone or betamethasone) mature the fetal lung, inducing the enzymes for surfactant synthesis and the genes for the surfactant proteins, increase anti-oxidant activity, and reduce oxidative stress.
Which is better dexamethasone or betamethasone?
Based on the results of this study and other similar works in this area, it can be concluded that dexamethasone has lower effect on AFI, BPP, and NST indexes respect to betamethasone and for this reason it is more preferred rather than betamethasone.
Which is the most important clinical indication for the use of surfactant in patients?
Clinical indications Surfactant replacement therapy should be considered in: neonates with clinical and radiographic evidence of RDS. neonates at risk of developing RDS (e.g. <32 weeks or low birth weight <1300g) neonates who are intubated, regardless of gestation, and requiring FiO2 >40%