Where are amides excreted
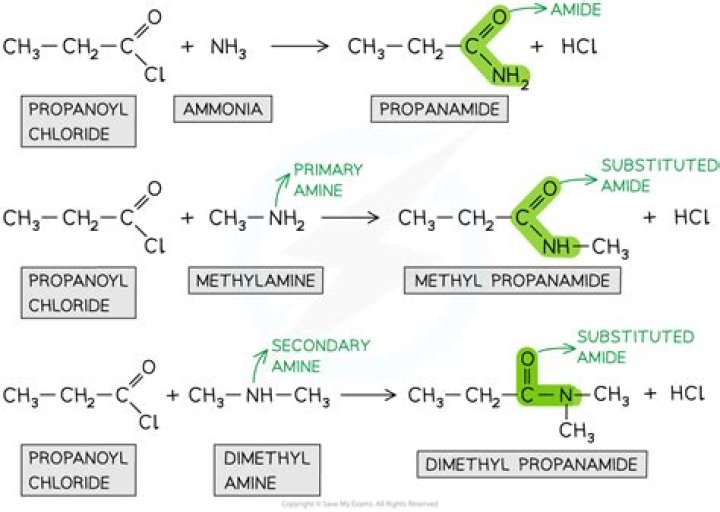
Amides are extremely stable in solution, while esters are unstable. The amino-esters are hydrolyzed in plasma by the enzyme pseudocholinesterase, whereas the amide compounds undergo enzymatic degradation in the liver and excretion in the urine.
Where is lidocaine metabolized?
Lidocaine is metabolized in the liver by the P450 3A4 isoenzyme, a member of the subfamily of P450 isoenzymes.
Where is Articaine metabolized?
Articaine is metabolized in the serum by plasma cholinesterase; although synthesis of cholinesterase is decreased in patients with liver diseases, fast hydrolysis is presumably preserved in their erythrocytes.
Which amide anesthetic agent is metabolized by the lungs before it reaches the liver?
Local Anesthetics Amides undergo enzymatic biotransformation primarily in the liver. The lungs may also extract lidocaine, bupivacaine, and prilocaine from circulation. Chloroprocaine is least likely to produce sustained elevation in blood levels because of very rapid hydrolysis in the blood.Which of the following is amide local Anaesthetic?
Lidocaine (lye’ do kane), bupivacaine (bue piv’ a kane) and ropivacaine (roe piv’ a kane) are commonly used local anesthetics that are chemically referred to as aminoethylamides or amide local anesthetics.
Is lidocaine processed in the liver?
Lidocaine is almost completely metabolised by dealkylation in the liver by CYP34A. The initial metabolite is monoethylglycinexylidie (MEGX). It is pharmacologically active, has a half-life of longer duration than that of lidocaine but is not as effective in blocking the sodium channel.
What is amide anesthetic?
Amide local anesthetics are commonly used for pain control during minor surgery. Local anesthesia causes a temporary loss of sensation, including pain, without depressing the consciousness. It acts within nerve fibers to inhibit the rapid inflow of sodium necessary for impulse generation.
Does lidocaine affect the liver?
Lidocaine metabolising capacity of the liver was irrespective of etiology of cirrhosis. It was also found that evaluation of elimination half-life of lidocaine is more closely related to the Child-Pugh’s staging of liver dysfunction than 15-minute MEGX concentration.Which local anesthetic is metabolized by plasma cholinesterase?
Two commonly used drugs—succinylcholine, a short-acting, depolarizing muscle relaxant used during intubation in general anesthesia, and the ester local anesthetics, such as procaine, chloroprocaine, tetracaine, and propoxycaine—are metabolized by the enzyme plasma cholinesterase.
Which amide anesthetic is metabolized in both the plasma and the liver?Because ropivacaine is an amide-type local anesthetic, it is metabolized by cytochrome P450 (P450) in the liver, and its elimination and plasma concentration can be dependent on the level of P450.
Article first time published onIs bupivacaine an amide?
The commonly used amide LAs include lidocaine, bupivacaine, ropivacaine, mepivacaine, and outside the United States, levobupivacaine. Articaine is an amide LA used primarily in dentistry. LAs are weak bases that exist in solution in both charged and uncharged forms.
What is the name of the only topical amide anesthetic currently on the dental market in the United States?
Articaine hydrochloride 4% (Septocaine) is an amide local anesthetic that has been used in Europe and other parts of the world for years and has now been approved for use in the United States. The only preparation available contains 1:100,000 epinephrine.
Is prilocaine an ester or amide?
Esters include benzocaine, chloroprocaine, cocaine, procaine, proparacaine, and tetracaine. The amides include articaine, bupivacaine, levobupivacaine, dibucaine, etidocaine, mepivacaine, prilocaine, ropivacaine, and finally, lidocaine.
Is Septocaine an ester or amide?
Septocaine is actually a hybrid of both an amide and an ester class anesthetic because of the presence of both an amide and an ester intermediate chain in its chemical composition.
Where is prilocaine metabolized?
Prilocaine is metabolized in both the liver and the kidney and excreted via the kidney.
Where is local anesthesia injected?
Epidural and spinal anaesthetics An epidural anaesthetic, often referred to as an epidural, is where a local anaesthetic is continually injected through a tube into an area of the lower back called the epidural space. A spinal anaesthetic is a single injection into a similar space in the back.
What is the most commonly used local anesthetic?
Lignocaine (lidocaine) is the most commonly used anaesthetic in the surgical setting. It is effective, acts rapidly and is relatively free from toxicity and sensitivity. It is available in many different forms, including topical applications (eg, EMLA® Cream and patches) and solutions for injection.
How are amides used in medicine?
For use in the treatment of duodenal ulcers, as a diuretic, and in the treatment of glaucoma, and may also be useful in the treatment of seizures associated with epilepsy.
Which is an amino amide derivative used as local anesthetic?
Commonly used amino amides include lidocaine, mepivacaine, prilocaine, bupivacaine, etidocaine, and ropivacaine and levobupivacaine.
What medicines contain amides?
- AneCream.
- AneCream5.
- articaine/epinephrine.
- bupivacaine.
- bupivacaine implant.
- bupivacaine liposome.
- Carbocaine.
- Citanest.
What is the functional group of amides?
Amides are compounds that consist of a carbonyl functional group which is connected to both an amine group and a hydrocarbon group (or hydrogen atom). A carbonyl functional group consists of a carbon atom which is double-bonded with an oxygen atom.
Is lidocaine metabolized in the kidney?
While lidocaine pharmacokinetics are not significantly altered in CKD, its clearance has been shown to be reduced in proportion to the degree of impairment in kidney function in patients not receiving hemodialysis [17].
How fast is lidocaine metabolized?
Lidocaine has a 90% hepatic metabolism, and the elimination half-life is 1.5 to 2 hours, which can be prolonged up to 3.5 fold in patients with severe liver disease.
What class of local anesthetic should be avoided in patients with liver insufficiency?
Considering general anesthesia in these patients, investigations showed that among the inhalation anesthetics, Halothane should be avoided because maintaining hepatic blood flow is critical in hepatic patients.
Which drug is metabolized by plasma cholinesterase?
Plasma cholinesterase is an enzyme which has importance to the anaesthetist primarily for its role in the metabolism of suxamethonium, although other anaesthetic related drugs that this enzyme metabolises are also increasingly important.
Which local anesthetic is metabolized by Pseudocholinesterase?
Ester local anesthetics are predominantly metabolized by pseudocholinesterase.
Which local anesthetic can cause methemoglobinemia?
Prilocaine, widely used local anesthetic, can cause methemoglobinemia in pediatric patients even in therapeutic doses.
Which local anesthetic is best for liver disease?
Thus, articaine seems to be the local anesthetic of first choice in tissues with suppurative inflammation, for adults, children (over 4), elderly, pregnant women, breastfeeding women, patients suffering from hepatic disorders and renal function impairment.
Can tramadol mess up your liver?
Introduction. Tramadol is an opioid analgesic used for the therapy of mild-to-moderate pain. Tramadol overdose can cause acute liver failure. Pharmacologic doses of tramadol has not been associated with cases of clinically apparent drug induced liver disease.
Is anesthesia hard on your liver?
Anesthesia reduces cardiac output, induces splanchnic vasodilation, and causes a 30-50% reduction in hepatic blood flow. This places the cirrhotic liver at additional risk for decompensation.
Is Novocaine an ester or amide?
It contains an ester linkage between the aromatic nucleus and the amino group. NOVOCAIN is available as sterile solutions in concentrations of 1% and 2% for injection via local infiltration and peripheral nerve block.



