Which drug should be avoided in patients with second degree heart block
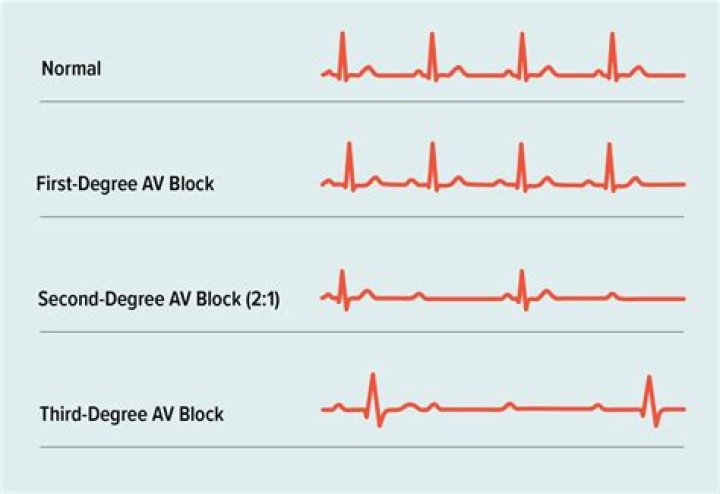
Second-degree AV block (Type 2) is clinically significant because this rhythm can rapidly progress to complete heart block. Atropine may be attempted if immediate TCP is not available or time is needed to initiate TCP. Atropine should not be relied upon and in the case of myocardial ischemia it should be avoided.
What medications cause 2nd degree heart block?
Common drugs that are known to cause AV block include beta-blockers, digoxin, calcium channel blockers, and many antiarrhythmic agents.
Why is atropine contraindicated in heart block?
When the vagus nerve is blocked, the SA node increases its rate of electrical discharge and this, in turn, results in the increased HR. Use atropine cautiously in the presence of myocardial ischemia and hypoxia because it increases oxygen demand on the heart and can worsen ischemia.
Do you give atropine for 2nd degree heart block?
Atropine can be used for immediate treatment of symptomatic second-degree atrioventricular (AV) block in the atrioventricular node (AVN). For block in the His-Purkinje system, atropine does not improve conduction and can actually precipitate third-degree AV block by increasing the sinus rate and AVN conduction.Can amiodarone be given in second-degree heart block?
Amiodarone therapy is contraindicated in patients with second- or third-degree heart block who do not have a pacemaker. Intravenously administered amiodarone causes heart block or bradycardia in 4.9 percent of patients and hypotension in 16 percent.
Can amlodipine cause AV block?
Amlodipine was changed to an angiotensin II receptor blocker (telmisartan) because amlodipine might have caused the AV block.
Can beta-blockers cause second-degree heart block?
In selected patients, combination therapy with a slow channel blocker and a beta blocker rarely causes second-degree AV block.
What is the treatment for 2nd degree AV block?
Treatments for second-degree heart block with symptoms include: Taking medicines to increase your heart rate in the short-term (acutely) to relieve symptoms. Stopping medicines, if they are causing the heart block. Getting a pacemaker.What drug is given after epinephrine?
Vasopressin should be effective in patients who remain in cardiac arrest after treatment with epinephrine, but there is inadequate data to evaluate the efficacy and safety of vasopressin in these patients (Class Indeterminate).
What is the drug of choice for bradycardia?The drug of choice is usually atropine 0.5–1.0 mg given intravenously at intervals of 3 to 5 minutes, up to a dose of 0.04 mg/kg. Other emergency drugs that may be given include adrenaline (epinephrine) and dopamine.
Article first time published onWhy does mobitz 2 worsen with atropine?
Atropine increases the conduction in the AV node. If the conduction block is infranodal (eg if the block is Mobitz II), an increase in AV nodal conduction by atropine only worsens the infranodal conduction delay and increases the AV block.
What are contraindications of atropine?
Atropine generally is contraindicated in patients with glaucoma, pyloric stenosis, thyrotoxicosis, fever, urinary tract obstruction and ileus.
What does amiodarone do to the heart?
Amiodarone belongs to the group of medicines known as antiarrhythmics. It works directly on the heart tissue and will slow the nerve impulses in the heart. This helps keep your heart rhythm normal.
Is amiodarone an AV nodal blocker?
In addition to procainamide, newly available parenteral antiarrhythmic agents for treatment of PSVT refractory to vagal maneuvers, adenosine, and AV nodal blocking agents include amiodarone, propafenone, flecainide, and sotalol.
What drugs should not be taken with amiodarone?
Other medications can affect the removal of amiodarone from your body, which may affect how amiodarone works. Examples include azole antifungals (such as itraconazole), cimetidine, cobicistat, protease inhibitors (such as fosamprenavir, indinavir), rifamycins (such as rifampin), St. John’s wort, among others.
Can amiodarone and digoxin be used together?
Digoxin and amiodarone are medications that are commonly used in patients with heart failure and/or atrial/ventricular arrhythmias. The coadministration of amiodarone and digoxin can increase the serum concentrations of digoxin and the risk for digoxin toxicity.
Is Amlodipine contraindicated in heart block?
Nifedipine and diltiazem should be used with caution in patients with heart failure because they may worsen outcomes. Amlodipine has been shown to be safe in heart failure.
What medications should be avoided in heart block?
- Nonsteroidal anti-inflammatory drugs. Aspirin.
- Calcium channel blockers.
- Drugs that may cause hyperkalemia.
- Trimethoprim-sulfamethoxazole.
- Antidepressants.
- Oral hypoglycemic agents. Thiazolidinediones. Metformin.
- Phosphodiesterase inhibitors. PDE-3 inhibitors. PDE-5 inhibitors.
- Antiarrhythmic agents.
Does atenolol cause heart block?
Atenolol can cause breathing difficulties in patients with asthma, chronic bronchitis, or emphysema. In patients with existing slow heart rates (bradycardias) and heart blocks (defects in the electrical conduction of the heart), atenolol can cause dangerously slow heart rates and even shock.
What calcium channel blockers cause heart block?
Beta-blockers and nondihydropyridine calcium channels antagonists (verapamil and diltiazem) are considered a common cause of acquired complete atrioventricular (AV) block in clinical practice. This is often stated axiomatically in reviews of the topic in major journals 1, 2and in textbooks of cardiology 3, 4, 5.
Which drug should be used with caution in a patient with first degree atrioventricular heart block?
Although first-degree AV block is not an absolute contraindication for administration of drugs such as calcium channel blockers, beta-blockers, digoxin, and amiodarone, extreme caution should be exercised in the use of these medications in patients with first-degree AV block.
When are calcium channel blockers contraindicated?
Calcium channel antagonists are also contraindicated in patients with known hypersensitivity to the drug or its components. Other contraindications include sick sinus syndrome (except in patients with an artificial pacemaker), severe hypotension, acute myocardial infarction, and pulmonary congestion.
Why epinephrine is given in anaphylactic shock?
Administer epinephrine intramuscularly every 5 to 15 minutes, in appropriate doses, as necessary, depending on the presenting signs and symptoms of anaphylaxis, to control signs and symptoms and prevent progression to more severe symptoms, such as respiratory distress, hypotension, shock, and unconsciousness.
What are the contraindications for epinephrine?
There are no absolute contraindications against using epinephrine. Some relative contraindications include hypersensitivity to sympathomimetic drugs, closed-angle glaucoma, anesthesia with halothane. Another unique contraindication to be aware of is catecholaminergic polymorphic ventricular tachycardia.
What is a second-degree type 2 heart block?
Second-degree AV block is a form of “incomplete” heart block, in which some, but not all, atrial beats are blocked before reaching the ventricles. Mobitz type II second-degree block is an old term, which refers to periodic atrioventricular block with constant PR intervals in the conducted beats.
What medications cause heart block?
Common drugs that induce atrioventricular (AV) block include beta-blockers, calcium channel blockers, antiarrhythmics, and digoxin. Withdrawal of the offending drugs is the first treatment for heart block.
What is the difference between Type 1 and Type 2 Second-degree heart block?
The hallmark of Mobitz type 1 block is the gradual prolongation of PR intervals before a block occurs. Mobitz type 2 block has constant PR intervals before blocks occur. Thus, if one can spot the gradual prolongation of PR intervals, Mobitz type 1 block should be diagnosed.
Does colchicine cause bradycardia?
Colchicine may increase the parasympathetic tone enough to cause sinus bradycardia and different degrees of heart block.
Which of the following drugs should be avoided in patients with irregular wide complex tachycardia?
It is so very critical to choose the right kind of medication once the decision is made to treat a patient with wide complex tachycardia. Calcium channel blockers (Diltiazem and verapamil) are strongly advised not to be used for fear of hemodynamic collapse, hypotension and cardiac arrest [4].
Can theophylline be used for bradycardia?
Effects of Theophylline Electrophysiological investigations showed that theophylline improves sinus node function in subjects with sinus bradycardia and enhances atrioventricular nodal conduction. The drug diminished the frequency and severity of bradycardia in newborn infants with spells of apnea-bradycardia.
What treatment may help a patient with a complete AV block?
Transcutaneous pacing is the treatment of choice for any symptomatic patient. All patients who have third-degree atrioventricular (AV) block (complete heart block) associated with repeated pauses, an inadequate escape rhythm, or a block below the AV node (AVN) should be stabilized with temporary pacing.



